Keywords:
By Nastya Yeska
Saliva-based tests are a reliable and proven method for measuring female hormone levels, as well as being highly accurate and painless for the patient.¹ This article takes you through five key steps to consider when setting up saliva-based testing for measuring and monitoring female hormone imbalance.

A hormone imbalance test for women can be based around saliva hormone testing.
1. Reassure yourself: saliva-based testing works
When measuring female hormones to discover underlying causes of female infertility, physicians need to be able to measure the levels of female sex hormones throughout the menstrual cycle. The same applies when solving other hormonal challenges, such as the personalized dosing required for hormone replacement therapy around menopause. This is because there are large differences in the concentration of hormones in each phase of the cycle, and in the timing of menstrual cycle events from woman to woman. Variations even exist across multiple cycles for an individual, including occasional non-ovulatory cycles.² You can read more about female steroid hormones in our testing guide, and in our introductory article to saliva testing.
Frequent serum sampling for hormone analysis would be invasive, inconvenient, and require skilled personnel to draw blood samples. However, saliva provides an excellent specimen for monitoring estradiol and progesterone levels across the menstrual cycle. It can even be self-collected at home on a daily basis. Samples can be stored in a freezer for at least a month, and also be subjected to repeated freezing and thawing without adverse effects on assay results.³ Other studies show that frozen samples can last for up to a year at –20°C, and possibly longer, without noticeable changes in the samples’ steroid hormone concentration.4
.jpeg?width=728&name=AdobeStock_166998197%20(1).jpeg)
Figure 1 shows a typical profile obtained from monitoring salivary progesterone and estradiol in self-collected whole saliva samples during the menstrual cycle, showing the peaks for estradiol and progesterone. This graph clearly demonstrates that even restricting sampling to every other day could result in skewed results, yet again proving the value of a simple, daily sampling method. It would be unrealistic to do venous blood sampling on a daily basis to obtain a similar result.
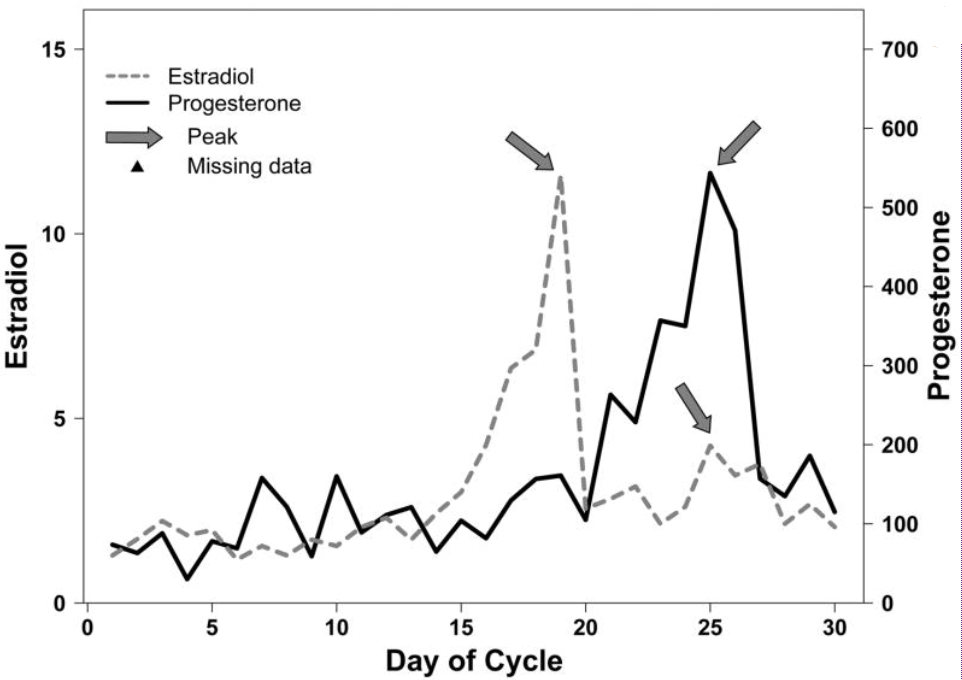
Figure 1. Representative patterns of salivary estradiol and progesterone levels across the normal menstrual cycle.¹
Not only are saliva tests extremely sensitive and accurate, they are also exceptionally reliable in measuring levels of free, bioavailable hormones. As we saw in the first article in this series, about 95-99% of steroid hormones circulating in the bloodstream are bound to carrier proteins. Since saliva contains unbound bioavailable hormones, salivary concentrations give a better representation of the actual circulating levels of free hormones.
2. Collect your sample: the essentials for saliva testing
Saliva-based testing begins with a reliable, standardized sampling technique, including a receptacle for the sample, so that it can be easily stored in a fridge or freezer. For maximum sensitivity, the testing lab must also ensure that the device used has been validated to minimize the interactions between the device surface and the salivary analyte being measured.
It is critical that the collection protocol used is compatible with the analyte to be tested. Some analytes can only be tested with samples collected by passive drool. Using a swab to measure these analytes can result in over- or under-recovery of the analyte being measured.
It is also recommended to use a swab that has been validated for the measurement of the analyte of interest. Some manufacturers have swabs that are specific to cortisol and have only been validated for the measurement of cortisol. Using this swab to measure another hormone, such as testosterone, can lead to erroneous results.
Polyethylene collection tubes should be avoided, since they may adsorb steroids. Polypropylene tubes are preferable in order to minimize steroid adsorption problems.6 The use of cotton-based materials can also be problematic. For example, although the use of Salivette® (Sarstedt) sampling tubes with cotton swabs is acceptable for measuring cortisol, results obtained for dehydroepiandrosterone (DHEA), testosterone, progesterone and estradiol using this method are spuriously high. This is thought to be due to the presence of plant sterols in the cotton, which cross-react in steroid immunoassays.7,8
Care should also be taken to avoid blood contamination in the sample, since this can skew the result. For example, elevated levels of testosterone are produced for at least 30 minutes after vigorous tooth-brushing.9
3. Test it out: check your ELISA works
Steroid hormones are present in relatively low concentrations in saliva, compared with serum, even if the hormone is mainly free rather than bound, so quantitative assays for salivary hormone assessment must be as sensitive as possible.
ELISA assays can provide the sensitivity required, but they must also be standardized within and between testing labs, ideally with an option to participate in inter-laboratory consistency testing as part of the quality control of the assay. In this way, a database of sample results can be built as numbers accumulate, and meta-analyses then carried out, moving saliva-based testing towards universal standardization.
It might also be useful to consider whether a given saliva-based ELISA test has been calibrated against mass spectroscopy (MS) results, since MS is the established reference method for hormone quantification. Having this calibration for a given test can give extra assurance, particularly when a lab is starting out with saliva-based ELISA testing, and needs empirical evidence that it is working effectively.10
Saliva-based ELISA tests must be standardized and reproducible in experimental terms: intra-assay, inter-assay, intra-lab, inter-lab, and batch-to-batch, with CVs within defined tolerance limits. Ideally, an ELISA inter-assay CV, whether between batches, people, or labs, should be <15%, and the intra-assay CV across triplicates should be <10%. Automation could be considered if enough tests are carried out, say in the 1000s or more per week, in terms of ELISA plates. Automated ELISA tests typically give results that are equivalent to an experienced manual worker, whilst removing much of the potential for human error.
4. Check the math: saliva testing is economically viable
When comparing costs that are unique to each method, saliva collection is 48% less costly than blood collection.11 In addition, saliva can be collected at home, and the samples easily stored without degradation, minimizing the risk of needing to repeat sample collections. This ease of collection is critical for measuring female hormone imbalance, where daily samples are often required, and the cyclical nature of the measurement means that any missing samples could further delay a potential diagnosis and treatment for another month.
Once sample collection is complete, additional costs will depend on the technology platform used (e.g. manual versus automated ELISA, and ELISA versus MS), although by far the greater cost will come from the clinical consultations and follow-up treatments, rather than from the tests themselves.
Saliva-based testing for female hormone imbalance is not routinely covered by insurance or public healthcare, although it may be part of a broader scheme to investigate defined conditions, such as infertility. In cases where women self-refer, for example when looking to relieve menopausal symptoms, it is worth noting that there is a plethora of tests available online, some of which are saliva-based, and others blood-based. These generally have a one-off, non-refundable cost, that includes a basic online consultation.
5. Diversify: use saliva testing for other applications too
Even if you find that saliva testing is relatively easy to set up in your lab, it is good to know that the effort put into optimizing it for your particular needs is not limited to the testing of female hormone levels. Saliva can be used to measure many other biomarkers, which means you can capitalize on the investment that you put into developing the infrastructure, adapting the workflow to include, for example, male hormone levels or other types of steroids.12 More information on how to go about this can be found in our saliva-based diagnostics guide.
To this end, saliva-based tests have already been developed in various other areas, including - but not limited to - sports medicine, psychology, and occupational medicine. For instance, high levels of cortisol are associated with stress and burnout, and cortisol was one of the first markers to be measured in saliva samples, making it a realistic target for measuring stress levels in the workplace.13 It is also worth noting that many labs that test for female hormone imbalance also check adrenal status as part of an overall hormone review, and therefore measure cortisol and DHEA levels in order to give a complete picture of a woman’s hormone status. In effect, there are many overlaps in the different hormonal pathways, as we saw in the first article of this series. However, the exact clinical application for which a specific test is relevant should always be considered, according to the individual test instructions.
In our final article, we will examine in more detail some of the technologies available for saliva-based hormone testing for women. Whether you are just starting out in this field, or adding to an existing infrastructure, you will then be well on the way to knowing how to diagnose and treat some of the most prevalent and emotive reproductive health issues in the world.
To read more about female steroid hormones download our testing guide.
References
1. Gandara, B. K., Leresche, L., & Mancl, L. (2007). Patterns of salivary estradiol and progesterone across the menstrual cycle. Annals of the New York Academy of Sciences 1098, 446-450. PubMed ID: https://pubmed.ncbi.nlm.nih.gov/17435149/ DOI:https://doi.org/10.1196/annals.1384.022
2. Becker, J. B., Arnold, A. P., Berkley, K. J., Blaustein, J. D., Eckel, L. A., Hampson, E., Herman, J. P., Marts, S., Sadee, W., Steiner, M., Taylor, J., & Young, E. (2005). Strategies and methods for research on sex differences in brain and behavior. Endocrinology, 146(4), 1650–1673. PubMed ID: https://pubmed.ncbi.nlm.nih.gov/15618360/ DOI: https://doi.org/10.1210/en.2004-1142
3. Gandara B., LeResche L., & Mancl L. (2006) Effects of repeated freeze-thaw in self-collected salivary hormone specimens. [abstract] J. Dent. Res. p. 1045.
4. Schultheiss, O. C., & Stanton, S. J. (2009). Assessment of salivary hormones. In E. Harmon-Jones & J. S. Beer (Eds.), Methods in social neuroscience (p. 17–44). Guilford Press.
5. Bellagambi, F.G., Lomonaco, T., Salvo, P., Vivaldi F., Hangouet, M., Ghimenti, S., Biagini, D., Di Francesco, F. & Fuoco, R. & Errachid, A. (2020). Saliva sampling: Methods and devices. An overview. Trends in Analytical Chemistry. Elsevier. Volume 124, March 2020, 115781 Elsevier ID: https://www.sciencedirect.com/science/article/abs/pii/S0165993619304182?via%3Dihub DOI: https://doi.org/10.1016/j.trac.2019.115781
6. Wood, Peter (2009) Salivary steroid assays - research or routine? Annals of clinical biochemistry 46 (3), 183-196. PubMed ID: https://pubmed.ncbi.nlm.nih.gov/19176642/ DOI: https://doi.org/10.1258/acb.2008.008208
7. Lewis John G. (2006). Steroid Analysis in Saliva: An overview. Clin Biochem Rev Vol 27, 139-146. PubMed ID: https://pubmed.ncbi.nlm.nih.gov/17268582/
8. Shirtcliff, E.A., Granger, D.A., Schwartz, E., & Curran, M.J. (2001). Use of salivary biomarkers in biobehavioral research: cotton-based sample collection methods can interfere with salivary immunoassay results. Psychoneuroendocrinology, 26:165–73. PubMed ID: https://pubmed.ncbi.nlm.nih.gov/11087962/ DOI: https://doi.org/10.1016/s0306-4530(00)00042-1
9. Kivlighan, K. T., Granger, D. A., Schwartz, E. B., Nelson, V., Curran, M., & Shirtcliff, E. A. (2004). Quantifying blood leakage into the oral mucosa and its effects on the measurement of cortisol, dehydroepiandrosterone, and testosterone in saliva. Hormones and behavior, 46(1), 39-46. PubMed ID: https://pubmed.ncbi.nlm.nih.gov/15215040/ DOI: https://doi.org/10.1016/j.yhbeh.2004.01.006
10. Stanczyk, F. Z., & Clarke, N. J. (2010). Advantages and challenges of mass spectrometry assays for steroid hormones. The Journal of steroid biochemistry and molecular biology, 121(3-5), 491–495. PubMed ID: https://pubmed.ncbi.nlm.nih.gov/20470886/ DOI: https://doi.org/10.1016/j.jsbmb.2010.05.001
11. https://blog.dnagenotek.com/blogdnagenotekcom/bid/86396/dna-from-saliva-vs-blood-who-wins-the-cost-battle Accessed 21 July 2020.
12. Yoshizawa, J. M., Schafer, C. A., Schafer, J. J., Farrell, J. J., Paster, B. J., & Wong, D. T. (2013). Salivary biomarkers: toward future clinical and diagnostic utilities. Clinical microbiology reviews, 26(4), 781–791. PubMed ID: https://pubmed.ncbi.nlm.nih.gov/24092855/ DOI: https://doi.org/10.1128/CMR.00021-13
13. van den Heuvel, L. L., Wright, S., Suliman, S., Stalder, T., Kirschbaum, C., & Seedat, S. (2019). Cortisol levels in different tissue samples in posttraumatic stress disorder patients versus controls: a systematic review and meta-analysis protocol. Systematic reviews, 8(1), 7. PubMed ID: https://pubmed.ncbi.nlm.nih.gov/30616687/ DOI: https://doi.org/10.1186/s13643-018-0936-x
Keywords:
About the author

Nastya Yeska
Nastya Yeska joined Tecan in 2017 as a product manager responsible for the Complementary medicine product portfolio, including Food intolerance and Saliva diagnostics. Nastya is part of Global Reagent Marketing & Support Department responsible for delivering ELISA solutions. In 2021, she changed her role to Integrated Marketing Manager.











